
In the treatment of trauma, IFS is different from traditional phase-oriented treatments. Instead of starting with building resources in clients before processing traumatic memories, it welcomes extreme symptoms from the onset, learns about their positive protective intentions and gets their permission to access the traumatic wounds. IFS also differs from traditional attachment focused therapies, both value the therapeutic relationship; however, IFS additionally supports the relationship between the client’s “Self” and their part as the primary healing agent.
Hailed by Dr. van der Kolk, the world’s leading expert in trauma, IFS is the treatment method that all clinicians should know. Nearly all clients with a trauma history have innate abilities that help them improve their mental health if they listen to their parts. IFS does just that. IFS is an evidence-based approach for clinicians working with traumatized clients. Once you see it in action, you’ll want to incorporate it into your practice.
Join IFS and trauma expert Frank Anderson, MD, colleague of Dr. Bessel van der Kolk and Dr. Richard Schwartz, in this transformational certificate training.
Clients will leave your office with skills to use outside the therapy room to help them master their emotions. This experiential training will show video demonstrations and include exercises and meditation techniques to use with your clients.
Treating Complex Trauma with Internal Family Systems (IFS)
Live Video Webcast

Today Only £349 (VAT Inclusive) — an unbelievable value!
Earn up to 15 CPD Hours—included in the price!
Interested in attending the live event in London? Click here to register for a seat with Dr. Frank Anderson

Frank Anderson, MD, completed his residency and was a clinical instructor in psychiatry at Harvard Medical School. He is both a psychiatrist and psychotherapist. He specialises in the treatment of trauma and dissociation and is passionate about teaching brain-based psychotherapy and integrating current neuroscience knowledge with the IFS model of therapy.
Dr. Anderson is the vice chair and director of the Foundation for Self Leadership. He is a trainer at the Center for Self Leadership with Richard Schwartz, PhD, and maintains a long affiliation with, and trains for, Bessel van der Kolk’s Trauma Center at Justice Resource Center in Boston, MA.
Dr. Anderson has lectured extensively on the Neurobiology of PTSD and Dissociation and wrote the chapter “Who’s Taking What” Connecting Neuroscience, Psychopharmacology and Internal Family Systems for Trauma in Internal Family Systems Therapy-New Dimensions. He co-authored a chapter on “What IFS Brings to Trauma Treatment in Innovations and Elaborations in Internal Family Systems Therapy” and recently co-authored Internal Family Systems Skills Training Manual.
Dr. Anderson maintains a private practice in Concord, MA, and serves as an Advisor to the International Association of Trauma Professionals (IATP).
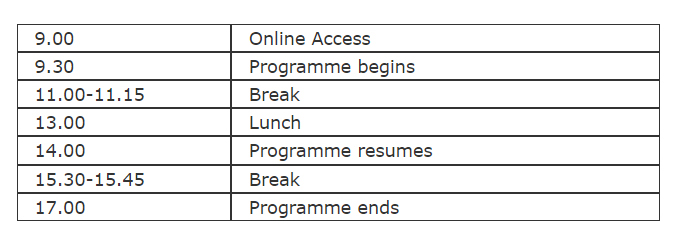
Webcast Schedule:
Objectives:
Upon completion of this workshop, participants will be able to:
- Integrate the IFS model into your clinical practice and accelerate the healing from complex trauma.
- Identify, specify and clarify the protective parts of clients with trauma histories to help with assessment and treatment planning.
- Offer an alternative view of symptoms and psychopathology, showing how client’s parts are actually trying to protect them from emotional pain and psychological pain.
- Demonstrate how IFS translates common comorbidities into parts language, showing a non-pathological perspective of mental health disorders.
- Communicate how IFS increases the therapist’s curious and compassionate self when working with clients who have trauma histories.
- Differentiate a therapeutic issue from a biological condition for better decision making in your clinical practice.
- Compare traditional attachment theory perspectives on healing to the IFS view (an internal attachment model) and learn to trust the clients’ internal relationship to heal their traumatic wounds.
- Understand how to respond to the extreme symptoms of trauma by determining if they are rooted in sympathetic activation or parasympathetic withdrawal.
- Demonstrate IFS specific therapeutic techniques that shift arousal and withdrawal, allowing quicker access to clients’ traumatic vulnerabilities.
- Develop a deep understanding of how neuroscience informs therapeutic decisions in IFS therapy.
- Integrate IFS with your current treatment approaches including EMDR, DBT, and Sensorimotor Psychotherapy.
- Compare IFS to traditional phase-oriented treatment and learn accelerated ways of accessing and healing traumatic wounds.
Cancellation Policy:
Booking terms and conditions for live events:
In the event you are unable to attend a workshop, conference or retreat please send a cancellation email to info@psychotherapyexcellence.com.
If you contact us before the event date, you may exchange your booking for the event recording (if available), a booking to attend another event, or a refund less a £50 cancellation fee. If you contact us the day of the event or after, you can receive the event recording or a gift certificate.
Occasionally, changes are made due to speaker availability, participant demand or unforeseen circumstances. While Psychotherapy Excellence will do everything possible to ensure participant satisfaction, Psychotherapy Excellence's liability is limited to the event fee only.
Treating Complex Trauma with Internal Family Systems (IFS)
Live Video Webcast
Today Only £349 (VAT Inclusive) — an unbelievable value!
Earn up to 15 CPD Hours—included in the price!
Interested in attending the live event in London? Click here to register for a seat with Dr. Frank Anderson